Introduction
Fibromyalgia and autoimmune diseases have long been subjects of medical debate due to their overlapping symptoms and complex causes. Fibromyalgia is characterized by widespread pain, fatigue, and cognitive issues, while autoimmune diseases occur when the immune system mistakenly attacks the body’s own tissues. Although fibromyalgia is not classified as an autoimmune disorder, research suggests a potential connection between immune dysfunction and fibromyalgia symptoms.
With ongoing studies exploring the links between these conditions, scientists are gaining new insights into their causes, diagnostic markers, and potential treatments. This article delves into the latest research on fibromyalgia and autoimmune diseases, shedding light on emerging theories and advancements in medical science.
1. Understanding the Link Between Fibromyalgia and Autoimmune Diseases
Overlapping Symptoms and Misdiagnoses
Both fibromyalgia and autoimmune diseases share symptoms such as chronic pain, fatigue, brain fog, and sleep disturbances. Conditions like lupus, rheumatoid arthritis, and multiple sclerosis can mimic fibromyalgia, leading to frequent misdiagnoses. Researchers are working to identify specific biomarkers that differentiate fibromyalgia from autoimmune conditions, improving diagnostic accuracy.
Immune System Dysfunction in Fibromyalgia
Recent studies suggest that fibromyalgia may involve immune system abnormalities, even though it is not officially classified as an autoimmune disease. Researchers have found that fibromyalgia patients exhibit higher levels of inflammatory cytokines—proteins that regulate immune responses. This has led to new theories that chronic inflammation and immune dysfunction could contribute to fibromyalgia symptoms.
2. The Role of Autoantibodies in Fibromyalgia
Groundbreaking Studies on Autoantibodies
A 2021 study published in The Journal of Clinical Investigation found that fibromyalgia patients had specific autoantibodies that could be linked to pain sensitivity. When researchers transferred these autoantibodies into mice, the animals developed fibromyalgia-like symptoms, including increased sensitivity to pain and muscle stiffness. This groundbreaking discovery suggests that fibromyalgia may have an immune-mediated component, paving the way for new treatment approaches.
Potential for Autoimmune Treatments
Since autoantibodies have been implicated in fibromyalgia, scientists are exploring whether immunosuppressive treatments commonly used for autoimmune diseases could help fibromyalgia patients. Some preliminary trials have tested medications like intravenous immunoglobulin (IVIG) and biologic drugs, showing potential benefits in reducing pain and fatigue.
3. Chronic Inflammation and Fibromyalgia
The Role of Neuroinflammation
Recent research highlights the presence of neuroinflammation in fibromyalgia patients. Studies using PET scans have detected increased levels of microglial activation in the brains of fibromyalgia sufferers. Microglia are immune cells in the nervous system that become overactive in response to injury or disease, leading to chronic pain and fatigue.
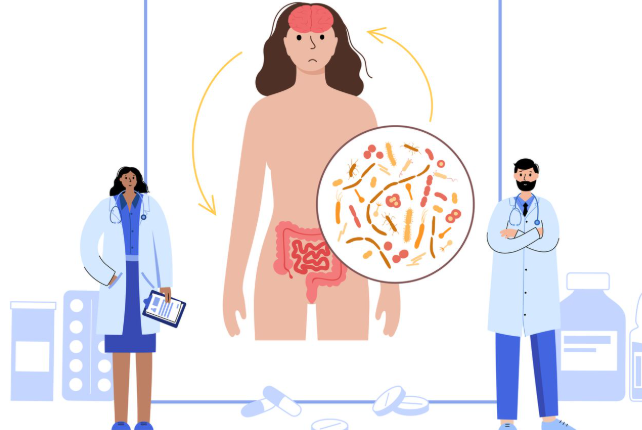
Gut Microbiome and Systemic Inflammation
Emerging studies suggest a link between gut health and fibromyalgia. Research published in Pain found that fibromyalgia patients had altered gut microbiota, with reduced levels of beneficial bacteria and an increase in pro-inflammatory species. Since the gut microbiome plays a critical role in immune regulation, imbalances may contribute to systemic inflammation and heightened pain sensitivity.
C-Reactive Protein (CRP) Levels and Fibromyalgia
While CRP is a common inflammatory marker used to diagnose autoimmune diseases, fibromyalgia patients often have slightly elevated but non-diagnostic CRP levels. This finding suggests that fibromyalgia involves low-grade inflammation that does not reach the levels seen in autoimmune diseases but still contributes to symptoms.
4. Emerging Diagnostic Tools for Fibromyalgia
Blood Tests and Biomarkers
Researchers are working on developing blood tests to diagnose fibromyalgia more accurately. Some promising biomarkers include:
- Altered levels of cytokines and chemokines (proteins involved in immune response)
- Specific autoantibodies that correlate with pain levels
- Metabolic changes detectable in blood samples
Although these tests are still in the experimental phase, they could revolutionize the way fibromyalgia is diagnosed in the future.
Advanced Imaging Techniques
Functional MRI (fMRI) and PET scans have shown that fibromyalgia patients have distinct brain activity patterns. These imaging tools reveal heightened pain processing in the central nervous system, confirming that fibromyalgia is a real, physiological condition rather than a psychological disorder.
5. New Treatment Approaches Based on Recent Research
Immunomodulatory Therapies
Since immune dysfunction appears to play a role in fibromyalgia, some researchers are investigating the use of immunomodulatory drugs. Early studies have explored:
- IVIG therapy, which has shown promise in reducing pain and fatigue
- TNF inhibitors, commonly used for rheumatoid arthritis, being tested for their effects on fibromyalgia symptoms
- Low-dose naltrexone (LDN), which modulates the immune response and has demonstrated positive results in small-scale fibromyalgia studies
Personalized Medicine Approaches
With advancements in genetic and biomarker research, personalized medicine is becoming a potential game-changer for fibromyalgia treatment. Scientists are working on tailoring treatments based on an individual’s immune profile, genetic predisposition, and metabolic markers.
Gut-Targeted Therapies
Since gut microbiome imbalances are linked to fibromyalgia, probiotics, prebiotics, and dietary interventions are being studied as potential treatments. Some trials suggest that correcting gut dysbiosis may reduce inflammation and improve fibromyalgia symptoms.
Non-Pharmacological Approaches
Recent research supports alternative therapies for fibromyalgia, including:
- Acupuncture, which has been shown to reduce pain sensitivity by modulating immune responses
- Cognitive-behavioral therapy (CBT), which helps manage pain perception and emotional distress
- Physical therapy, which improves mobility and reduces stiffness by targeting inflammation
Conclusion
The latest research on fibromyalgia and autoimmune diseases is uncovering important connections between immune dysfunction, chronic inflammation, and nervous system hypersensitivity. While fibromyalgia is not officially classified as an autoimmune disease, growing evidence suggests that immune system abnormalities play a significant role in its development and progression.
With advancements in diagnostic tools, personalized medicine, and immunomodulatory treatments, there is hope for more effective management strategies in the near future. Continued research will help refine our understanding of fibromyalgia, potentially leading to better treatments and improved quality of life for those affected by this challenging condition.

Click Here to Visit the Store and find Much More….
For More Information Related to Fibromyalgia Visit below sites:
References:
Fibromyalgia Contact Us Directly
Click here to Contact us Directly on Inbox
Official Fibromyalgia Blogs
Click here to Get the latest Chronic illness Updates
Fibromyalgia Stores